You love cycling. The freedom, the fitness benefits, the mental clarity. But lately, you’ve noticed something concerning: a dull ache in your scrotum after long rides, or perhaps visible swelling that wasn’t there before.
If you’ve been diagnosed with varicocele, or suspect you might have one, you’re probably wondering whether your bike is making things worse. It’s a valid concern that brings many men to their urologist’s office each year.
Here’s what you need to know: cycling doesn’t directly cause varicocele. However, prolonged saddle pressure and specific riding conditions can worsen symptoms in men who already have this condition. The good news? With proper adjustments and awareness, most cyclists can continue riding without significant problems.
This article breaks down the relationship between cycling and testicular vein health, backed by current research. For a complete overview of varicocele causes and treatment options, see our complete varicocele guide.


What Is Varicocele? A Quick Refresher
Varicocele refers to enlarged veins within the scrotum, specifically in the pampiniform plexus. This network of veins drains blood from the testicles. When the valves inside these veins malfunction, blood pools and causes the veins to swell.
Quick Facts About Varicocele
| Aspect | Details |
|---|---|
| Prevalence | Affects 15-20% of all men |
| Common side | 85-90% occur on the left side |
| Typical age of diagnosis | 15-35 years old |
| Main symptoms | Dull ache, heaviness, visible swelling |
| Fertility impact | Present in 40% of men with primary infertility |
Think of varicocele like varicose veins in the legs, but located in the scrotum. The condition develops due to valve weakness, not external injury. This distinction matters when we discuss cycling’s role.
Does Cycling Cause Varicocele?
The direct answer: No, cycling does not cause varicocele.
Varicocele develops from internal valve dysfunction in the testicular veins. These valves fail for anatomical and genetic reasons, not because of external pressure from a bike seat. Research published in BJU International confirms that varicocele formation relates to venous valve incompetence and the angle at which the left testicular vein connects to the renal vein.
However, this doesn’t mean cycling has zero impact on your testicular vein health.
What Cycling Actually Does
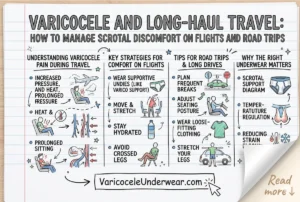
Prolonged cycling creates specific conditions that can affect the scrotal area:
- Direct perineal pressure: The saddle compresses blood vessels and nerves
- Increased scrotal temperature: Close contact with the seat traps heat
- Vibration and friction: Road surfaces transmit constant microtrauma
- Prolonged venous pressure: Static seated position can impair blood return
A 2021 study examining 100 male cyclists found that those riding more than 200 km per week showed higher rates of scrotal discomfort compared to recreational riders. The study didn’t find increased varicocele formation, but symptom aggravation was notable.
Can Cycling Make Varicocele Worse?
Yes, cycling can worsen varicocele symptoms in some men. This doesn’t mean the condition itself is progressing, but rather that symptoms become more noticeable or bothersome.
How Cycling Aggravates Symptoms
| Factor | Effect on Varicocele |
|---|---|
| Saddle pressure | Compresses venous drainage pathways |
| Heat accumulation | Worsens venous dilation, increases discomfort |
| Prolonged sitting | Impairs venous return to the heart |
| Vibration | May increase inflammation and pain sensitivity |
| Tight cycling shorts | Can either help (compression) or hurt (heat trapping) |
Case Study: Daniel, 42, an avid road cyclist averaging 150 miles per week, came to his urologist with worsening left scrotal pain after rides. He had a known Grade II varicocele diagnosed years earlier that had been asymptomatic. After implementing saddle changes and reducing ride duration, his symptoms improved by approximately 70% within six weeks.
Signs Your Cycling Is Aggravating Your Varicocele
Watch for these patterns:
- Pain or heaviness that specifically appears during or after rides
- Symptoms that resolve on non-cycling days
- Visible swelling that increases after long rides
- Discomfort that correlates with ride distance or duration
If you notice these patterns, your cycling setup likely needs attention. The condition itself isn’t worsening, but your riding conditions are triggering symptoms.
Bike Seat Pressure and Testicular Blood Flow
The relationship between saddle design and genital blood flow is well-documented in cycling medicine. Understanding this helps explain why some cyclists experience more problems than others.
The Anatomy of Saddle Pressure
When you sit on a traditional bike seat, your body weight concentrates on a small area. The perineum (the area between your scrotum and anus) bears significant load. This region contains:
- The pudendal artery and nerve
- Venous drainage pathways from the testicles
- Portions of the urethra
- Erectile tissue
Research from the National Institutes of Health shows that traditional narrow bike seats can reduce penile blood flow by up to 70% during cycling. While this research focused on erectile function, the same pressure affects testicular venous drainage.
Saddle Types and Their Impact
| Saddle Type | Pressure Distribution | Impact on Varicocele Symptoms |
|---|---|---|
| Traditional narrow | Concentrated on perineum | Higher symptom aggravation |
| Noseless/cutout | Shifted to sit bones | Reduced venous compression |
| Wide cushioned | Distributed broadly | Variable, depends on fit |
| Split/channel design | Perineal pressure relief | Generally symptom-friendly |
Dr. Irwin Goldstein, a urologist specializing in cycling-related issues, has noted that saddle choice significantly affects genital blood flow. Cutout and noseless designs reduce perineal pressure by 50-70% compared to traditional saddles.
How to Cycle Safely with Varicocele
Having a varicocele doesn’t mean you need to quit cycling. With appropriate modifications, most men can continue riding comfortably.
Bike Setup Modifications
Saddle adjustments:
- Choose a saddle with a center cutout or channel
- Ensure proper saddle width matches your sit bone measurement
- Level the saddle or tilt the nose slightly downward (1-3 degrees)
- Set saddle height so your knee has a slight bend at the bottom of the pedal stroke
Position changes:
- Raise handlebars to reduce forward lean onto the perineum
- Consider a more upright riding position
- Stand on the pedals every 10-15 minutes during long rides
Equipment upgrades:
- Use padded cycling shorts with quality chamois
- Consider wearing supportive underwear designed for varicocele underneath cycling shorts for additional support
- Install a suspension seatpost to reduce vibration
Riding Habit Changes
| Recommendation | Reasoning |
|---|---|
| Take standing breaks every 10-15 minutes | Relieves sustained pressure |
| Limit continuous ride time initially | Allows symptom assessment |
| Choose smooth surfaces when possible | Reduces vibration trauma |
| Avoid riding in extreme heat | Minimizes scrotal temperature elevation |
| Stay hydrated | Supports healthy blood viscosity |
Case Study: Marcus, 28, a competitive mountain biker with Grade II varicocele, worked with a bike fitter to optimize his setup. Key changes included switching to a cutout saddle, adjusting saddle angle, and adding a dropper post for more frequent position changes. He reported 80% symptom reduction while maintaining his training volume.
Best Bike Seats for Varicocele: What to Look For
Saddle selection can significantly affect your comfort level when cycling with varicocele. Here’s what matters most.
Key Features for Varicocele-Friendly Saddles
Center cutout or channel:
This design removes pressure from the perineum entirely. Look for cutouts that extend from the nose through the center of the saddle.
Appropriate width:
Sit bones should rest on the padded portions of the saddle, not the edges. Most bike shops can measure your sit bone width.
Moderate padding:
Excessive padding can actually increase pressure by allowing your body to sink in. Firm but supportive padding works best.
Proper length:
Shorter saddles reduce contact area and often decrease pressure on sensitive regions.
Saddle Comparison for Cyclists with Varicocele
| Feature | Traditional Saddle | Cutout Saddle | Noseless Saddle |
|---|---|---|---|
| Perineal pressure | High | Low to moderate | Very low |
| Stability | High | High | Moderate |
| Learning curve | None | None | Several rides |
| Price range | $30-150 | $50-300 | $60-250 |
| Recommended for varicocele | No | Yes | Yes |
Popular saddle brands offering effective cutout designs include Specialized (Power series), ISM, SMP, and Ergon. A professional bike fit can help determine which specific model suits your anatomy and riding style.
Cycling Gear That Protects Testicular Health
Beyond the saddle, other equipment choices affect your comfort when cycling with varicocele.
Cycling Shorts Selection
Quality cycling shorts provide:
- Compression that supports scrotal position
- Chamois padding that reduces friction
- Moisture-wicking fabric that controls temperature
However, some cyclists find that standard cycling shorts trap too much heat, worsening varicocele symptoms. If this applies to you, consider:
- Shorts with mesh ventilation panels
- Lighter weight chamois options
- Layering supportive underwear beneath looser shorts for casual rides
Supportive Base Layers
Wearing supportive underwear specifically designed for varicocele can add an extra layer of protection during cycling. These garments provide consistent compression that helps maintain testicular position and may improve venous drainage during activity. For trail riding or shorter commutes where cycling shorts aren’t necessary, this option offers targeted support.
When to Take a Break from Cycling
Sometimes the best approach is temporary rest. Knowing when to pause helps prevent symptom escalation.
Signs You Should Stop Cycling Temporarily
- Persistent pain that doesn’t resolve within 24-48 hours after riding
- New or worsening testicular swelling
- Numbness in the genital area during or after rides
- Pain that interferes with daily activities
- Symptoms that progress despite equipment modifications
Alternative Activities During Recovery
If you need to take a cycling break, these activities maintain fitness while giving your varicocele symptoms time to settle:
- Swimming (excellent for varicocele due to horizontal position and cool water)
- Elliptical training
- Upper body strength training
- Walking or light jogging
- Rowing (in moderation)
Most men can return to cycling after symptoms improve, especially with proper equipment adjustments in place.
Does Cycling Affect Fertility with Varicocele?
This question concerns many cyclists, particularly those trying to conceive. The answer involves several factors.
What Research Shows
According to Mayo Clinic, varicocele affects fertility primarily through elevated scrotal temperature and impaired blood flow. Cycling adds to both these factors during riding.
A study published in Fertility and Sterility found that cyclists who rode more than 5 hours per week showed lower sperm concentration compared to non-cyclists. However, this effect was modest and didn’t necessarily prevent conception.
Practical Recommendations for Cyclists Trying to Conceive
| Situation | Recommendation |
|---|---|
| Actively trying to conceive | Limit rides to under 2 hours |
| Undergoing fertility treatment | Discuss cycling with your reproductive endocrinologist |
| Known varicocele affecting sperm | Consider temporary cycling reduction |
| Post-varicocelectomy | Follow your surgeon’s return-to-activity guidelines |
Cooling strategies matter: Taking breaks, wearing breathable gear, and avoiding riding in extreme heat all help protect sperm production.
Professional Cyclists and Varicocele: What We Know
Professional cycling demands thousands of hours in the saddle annually. How do elite athletes manage varicocele?
Insights from Elite Cycling
Professional cyclists undergo regular health monitoring that includes reproductive health assessments. While specific data is limited due to privacy concerns, sports medicine specialists report that:
- Varicocele rates among professional cyclists appear similar to the general population
- Equipment optimization is standard practice in elite cycling
- Many professionals use custom-molded saddles designed for their anatomy
- Team physicians monitor for saddle-related health issues proactively
The key takeaway: even at extreme training volumes, proper equipment and attention to symptoms allow athletes to compete successfully.
Frequently Asked Questions
How long can I cycle with varicocele before problems start?
Symptom onset varies significantly between individuals. Some men ride for hours without issues, while others notice discomfort after 30-45 minutes. Factors include your varicocele grade, saddle design, riding position, and personal anatomy. Start with shorter rides and gradually increase duration while monitoring symptoms. If discomfort develops, that’s your signal to take breaks or adjust your setup rather than push through.
Should I stop cycling after varicocele surgery?
Your surgeon will provide specific recovery timelines, but most men need to avoid cycling for 2-4 weeks after microsurgical varicocelectomy. When you return, start with short, easy rides on smooth surfaces. Avoid intense efforts or rough terrain for 4-6 weeks post-surgery. Return to full training volume gradually over 6-8 weeks. Wearing supportive underwear during early return to cycling can provide additional comfort.
Can a bike seat cause permanent testicular damage?
A properly fitted bike seat does not cause permanent testicular damage. However, chronic perineal pressure from poorly designed or improperly positioned saddles can contribute to temporary erectile issues and may aggravate existing varicocele symptoms. These effects are typically reversible with equipment changes and rest. If you experience persistent numbness or pain, stop riding and consult a urologist before continuing.
Final Takeaways for Cyclists with Varicocele
Cycling and varicocele can coexist. The key lies in paying attention to your body and making smart equipment choices.
What works:
- Cutout or noseless saddle designs
- Proper bike fit with appropriate saddle height and angle
- Regular standing breaks during rides
- Supportive, breathable cycling gear
- Monitoring symptoms and adjusting as needed
What to avoid:
- Traditional narrow saddles that concentrate perineal pressure
- Pushing through pain or ignoring symptoms
- Excessive heat exposure during rides
- Ignoring equipment as a potential cause of symptoms
If your varicocele symptoms significantly limit your riding despite these modifications, discuss treatment options with a urologist. Modern surgical techniques offer excellent outcomes with quick recovery times, getting most men back on their bikes within weeks.
Have questions about cycling with varicocele? Share your experience in the comments or consult a sports medicine physician for personalized guidance.