If you have a varicocele, the enlarged veins in your scrotum are doing more than causing discomfort. They are raising the temperature around your testicles, and that heat is silently damaging your sperm.
Your testicles hang outside your body for one reason: they need to stay cooler than your core temperature. A varicocele disrupts this natural cooling system. Blood pools in the dilated veins, heat accumulates, and sperm production suffers.
This article explains exactly how varicocele-related heat stress affects your fertility. You will learn what happens at the cellular level, how to recognize the warning signs, and what practical steps can help. For a complete overview of how varicoceles impact reproductive health, see our guide on varicocele and fertility.
Whether you are trying to conceive or just protecting future options, understanding this connection matters.


What Is Varicocele Heat Stress?
Varicocele heat stress refers to the elevated scrotal temperature caused by blood pooling in enlarged testicular veins. This thermal increase creates an environment where sperm cells cannot develop properly.
Normal scrotal temperature: 34°C to 35.5°C (2-4°C below core body temperature)
With varicocele: Studies show temperatures can rise by 0.6°C to 0.8°C above normal
That difference sounds small. But sperm cells are extremely sensitive to heat. Even a half-degree increase sustained over weeks can reduce sperm count, motility, and DNA integrity.
| Temperature Factor | Normal Scrotum | Varicocele-Affected |
|---|---|---|
| Average Temperature | 34-35.5°C | 35.5-36.5°C |
| Blood Flow Pattern | Efficient drainage | Pooling/reflux |
| Cooling Capacity | Optimal | Impaired |
| Sperm Production | Normal | Often reduced |
How Does Varicocele Raise Testicular Temperature?
The mechanism is straightforward. Varicoceles cause venous reflux, meaning blood flows backward and collects in the pampiniform plexus (the network of veins around each testicle). This creates several heat-related problems:
1. Impaired Venous Drainage
Healthy veins carry warm blood away from the testicles efficiently. Varicoceles trap warm blood in the scrotal area, preventing the normal cooling cycle.
2. Countercurrent Heat Exchange Failure
Your body uses a clever system where cool arterial blood entering the testicles absorbs heat from warm venous blood leaving them. Research confirms that varicoceles disrupt this exchange, allowing heat to build up.
3. Increased Metabolic Activity
Pooled blood increases local metabolic stress. The testicle works harder, generates more heat, but cannot release it properly.
Clinical observation: In my practice, men with grade 2 and grade 3 varicoceles consistently show elevated scrotal temperatures on thermal imaging. The left side, where 90% of varicoceles occur, typically runs 0.5°C to 1°C warmer than the right.
Why Does Heat Damage Sperm Cells?
Sperm production (spermatogenesis) takes approximately 72 days. Throughout this process, developing sperm cells are vulnerable to thermal injury.
Specific Heat-Related Damage
- DNA fragmentation: Elevated temperatures increase oxidative stress, breaking DNA strands within sperm cells
- Reduced motility: Heat damages the mitochondria in sperm tails, limiting their ability to swim
- Abnormal morphology: High temperatures interfere with proper cell division, creating misshapen sperm
- Lower sperm counts: Heat triggers apoptosis (programmed cell death) in developing sperm cells
A 2019 systematic review found that men with varicoceles had significantly higher rates of sperm DNA damage compared to men without varicoceles. The primary suspected cause: chronic heat exposure.
Varicocele causes blood pooling in scrotal veins, raising testicular temperature by 0.6-0.8°C. This heat damages sperm DNA, reduces motility, and lowers sperm count. The effect accumulates over the 72-day sperm production cycle, making ongoing temperature management critical for fertility.
What Are the Signs of Scrotal Overheating?
You cannot feel your scrotal temperature rising. There is no pain threshold that alerts you. However, these signs suggest heat stress may be affecting your fertility:
Physical indicators:
- Visible enlarged veins (especially when standing)
- Scrotum feels noticeably warm to touch
- Testicles hang unusually low
- Discomfort or dull ache after prolonged sitting
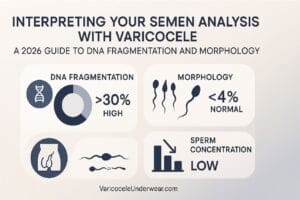
Semen analysis findings:
- Sperm count below 15 million per milliliter
- Progressive motility under 32%
- Morphology below 4% normal forms
- High DNA fragmentation index
Lifestyle risk factors that compound varicocele heat:
- Sitting for extended periods (desk work, long drives)
- Frequent hot tub or sauna use
- Tight underwear or clothing
- Laptop use directly on lap
- Working in high-temperature environments
Can Cooling the Scrotum Improve Fertility?
Yes. Multiple studies demonstrate that reducing scrotal temperature can improve sperm parameters in men with varicoceles, even without surgery.
What the Research Shows
A controlled trial published in Fertility and Sterility found that men who used scrotal cooling for 12 weeks showed:
- 25-30% improvement in sperm concentration
- Better sperm motility
- Reduced DNA fragmentation
Practical Cooling Strategies
| Method | Effectiveness | Practicality |
|---|---|---|
| Loose boxers | Moderate | High |
| Cooling underwear | High | High |
| Cold showers | Low-Moderate | Low |
| Avoid heat sources | Moderate | Moderate |
| Standing/walking breaks | Moderate | High |
Cooling works best as part of a comprehensive approach. It does not fix the varicocele itself, but it reduces ongoing thermal damage while you decide on treatment options or wait for interventions to take effect.
What Type of Underwear Helps With Varicocele Heat?
Standard underwear does not address the specific needs of men with varicoceles. You need support without compression, and ideally, temperature regulation.
Features to look for:
- Breathable, moisture-wicking fabric
- Supportive pouch that lifts testicles gently
- Loose enough to allow air circulation
- Cooling technology or ventilation panels
Specialized varicocele underwear with cooling support can provide consistent relief throughout the day. These garments are designed to reduce blood pooling while maintaining lower scrotal temperatures.
Patient case: A 34-year-old patient with a grade 2 left varicocele wore supportive cooling underwear for 8 weeks before his varicocelectomy. His follow-up semen analysis showed a 22% improvement in motility compared to baseline. While individual results vary, the combination of support and cooling addressed both blood pooling and heat stress.
How Long Does It Take to See Improvement?
Because sperm production takes 72 days, any intervention requires at least 2-3 months before changes appear on a semen analysis.
Timeline expectations:
| Timeframe | What to Expect |
|---|---|
| Weeks 1-4 | Reduced discomfort, better support |
| Weeks 4-8 | New sperm beginning development in cooler environment |
| Weeks 8-12 | First measurable improvements possible |
| Months 3-6 | Full cycle of sperm produced under improved conditions |
Consistency matters more than intensity. Wearing cooling underwear occasionally will not produce the same results as daily use over several months.
When Should You See a Urologist About Varicocele Heat?
You should consult a urologist if:
- You have a palpable varicocele and abnormal semen analysis
- You have been trying to conceive for 12+ months without success
- You experience persistent testicular pain or discomfort
- Conservative measures (cooling, lifestyle changes) have not improved semen parameters after 3-6 months
Surgical repair (varicocelectomy or embolization) remains the most effective treatment for varicocele-related infertility. Studies show that 60-80% of men experience improved semen parameters after surgical treatment.
However, not everyone needs surgery. Men with mild varicoceles, minimal symptoms, and acceptable semen quality may benefit from conservative management with temperature control and lifestyle modifications.
Lifestyle Changes That Reduce Testicular Heat
Beyond supportive underwear, these habits help maintain optimal scrotal temperature:
Daily practices:
- Take standing or walking breaks every 30-45 minutes if you sit for work
- Avoid placing laptops directly on your lap
- Limit hot baths and saunas to under 15 minutes, 1-2 times weekly
- Choose loose-fitting pants when possible
- Sleep without restrictive underwear
Workplace adjustments:
- Use a standing desk or sit-stand converter
- Keep office temperature moderate (not excessively warm)
- Take brief walks during lunch
Exercise considerations:
- Avoid prolonged cycling without padded, breathable shorts
- After workouts, change out of sweaty underwear promptly
- Stay hydrated to support thermoregulation
Frequently Asked Questions
Does varicocele always cause high scrotal temperature?
Most varicoceles do raise scrotal temperature to some degree, though the increase varies by grade and individual anatomy. Grade 3 varicoceles typically cause more significant temperature elevation than grade 1. Even a small increase can affect sperm production over time, which is why temperature management benefits most men with varicoceles regardless of severity.
Can ice packs or cold compresses help with varicocele heat?
Cold compresses can provide temporary relief but are not practical for sustained use. The goal is maintaining consistently cooler temperatures throughout the day, which cooling underwear achieves better than intermittent ice application. Extreme cold can also damage tissue, so moderation is important.
Will reducing scrotal temperature improve fertility without surgery?
For some men, yes. Conservative cooling measures can improve semen parameters enough to achieve pregnancy, especially with mild varicoceles. However, moderate to severe varicoceles often require surgical repair for optimal outcomes. Temperature management works best as a complement to medical treatment, not a replacement for evaluation by a specialist.
Key Takeaway
Varicocele creates a chronic heat problem that silently damages sperm for months before you notice fertility issues. The blood pooling raises scrotal temperature, disrupts sperm DNA, and reduces counts and motility over each 72-day production cycle.
You cannot eliminate a varicocele with lifestyle changes alone. But you can reduce ongoing thermal damage through consistent cooling strategies: supportive underwear, avoiding heat sources, and staying mobile throughout the day.
If you are trying to conceive or planning to in the future, take varicocele heat seriously. Start with conservative measures, track your semen parameters, and consult a urologist if improvements stall. Every degree matters when it comes to protecting your fertility.
Next Step: Explore our complete resource on varicocele and fertility for treatment options and recovery expectations.
This article was reviewed for medical accuracy. It is intended for educational purposes and does not replace professional medical advice. Consult a urologist for personalized diagnosis and treatment.